Slipped Disc Treatment Singapore – Non-Surgical Relief
Back pain that radiates down your leg, numbness in your feet, or sharp pain after sitting at your desk are not just inconveniences. These may be signs of a slipped disc, one of the most common and undertreated spinal conditions in Singapore.
At Elite Spine Centres, our expert chiropractors provide evidence-based slipped disc treatment in Singapore using a comprehensive, non-surgical approach that addresses the root cause, not just the pain. Most patients experience meaningful relief within weeks, without medication or surgery.
What Exactly is a Slipped Disc?
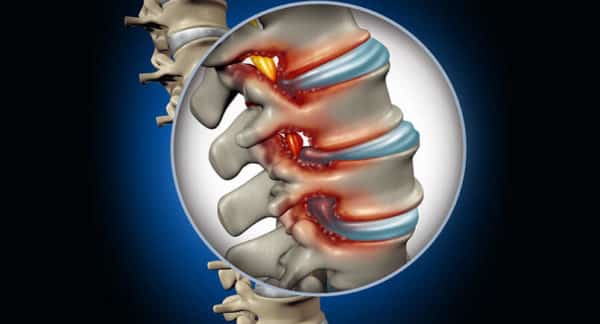
Your spine is made up of vertebrae separated by cushion-like discs. Each disc has a tough outer ring (the annulus fibrosus) encasing a soft, gel-like centre (the nucleus pulposus). When the outer layer weakens, tears, or is placed under too much stress, the inner material can push outward, pressing on nearby nerves. This is what we call a slipped, herniated, bulging, or prolapsed disc.
The most commonly affected areas are the lower back (lumbar spine) and the neck (cervical spine), as these regions bear the most strain from daily movement and postural habits.
Causes of a Slipped Disc
In most cases, a slipped disc is not caused by a single dramatic event. It builds up over time. Common contributing factors include:
Accumulated stress over time:
- Prolonged sitting with poor posture, whether at a desk or on your phone
- Repetitive bending, twisting, or heavy lifting at work
- Age-related disc degeneration (risk increases significantly from your 30s onward)
- Obesity or a sedentary lifestyle placing extra load on the spine
- Poor spinal alignment or mobility, often present for years before symptoms appear
Acute injuries:
- Whiplash or a hard landing on the back
- Sports injuries or awkward movements
- Lifting heavy objects without bending the knees
Many patients are surprised to learn their disc was already compromised before a seemingly minor incident triggered the pain.

Symptoms of a Slipped Disc
Disc pain treatment often begins with recognising the signs. Symptoms vary depending on the location of the herniation and whether a nerve is affected:
- Lower back pain or neck pain, sharp or dull
- Pain that radiates down the leg (often mistaken for sciatica) or down the arm
- Tingling or numbness in the shoulders, arms, hands, legs, or feet
- Muscle weakness affecting grip or leg stability
- Difficulty straightening the back
- Pain that worsens with prolonged sitting, standing, walking, or coughing
If left untreated, a slipped disc can lead to more serious complications including sciatica, chronic neuropathy, or in rare cases, cauda equina syndrome, which requires emergency surgery.
As Seen In
Our Slipped Disc Treatment Approach
At Elite Spine Centres, we use our signature Functional Correction Method (FCM), a whole-body, non-surgical treatment system developed specifically to treat the cause and symptoms of disc conditions. Your treatment plan is tailored to your age, lifestyle, pain levels, and recovery goals.
Treatment may include a combination of:
Spinal Decompression – Non-surgical spinal decompression (NSSD) gently reduces pressure on the affected disc, allowing healing nutrients and hydration to re-enter the disc tissue and gradually reducing the bulge.
Chiropractic Care – Precise spinal adjustments restore alignment, improve joint mobility, and reduce nerve irritation without invasive procedures.
Rehabilitative Exercises – Customised stretching and strengthening exercises rebuild the core and spinal support muscles to protect against recurrence.
Shockwave Therapy – Radial shockwave therapy reduces deep tissue inflammation and accelerates soft tissue recovery.
Laser Therapy – Low-level laser therapy (LLLT) supports cellular healing and helps manage pain in more chronic or inflamed cases.
Posture and Ergonomic Guidance – We identify the daily habits and postural patterns contributing to your condition and give you practical strategies for long-term posture correction.
This combination approach means our patients achieve more complete recovery in less time, with a significantly reduced chance of relapse compared to single-modality treatment.
What to Expect at Your First Visit
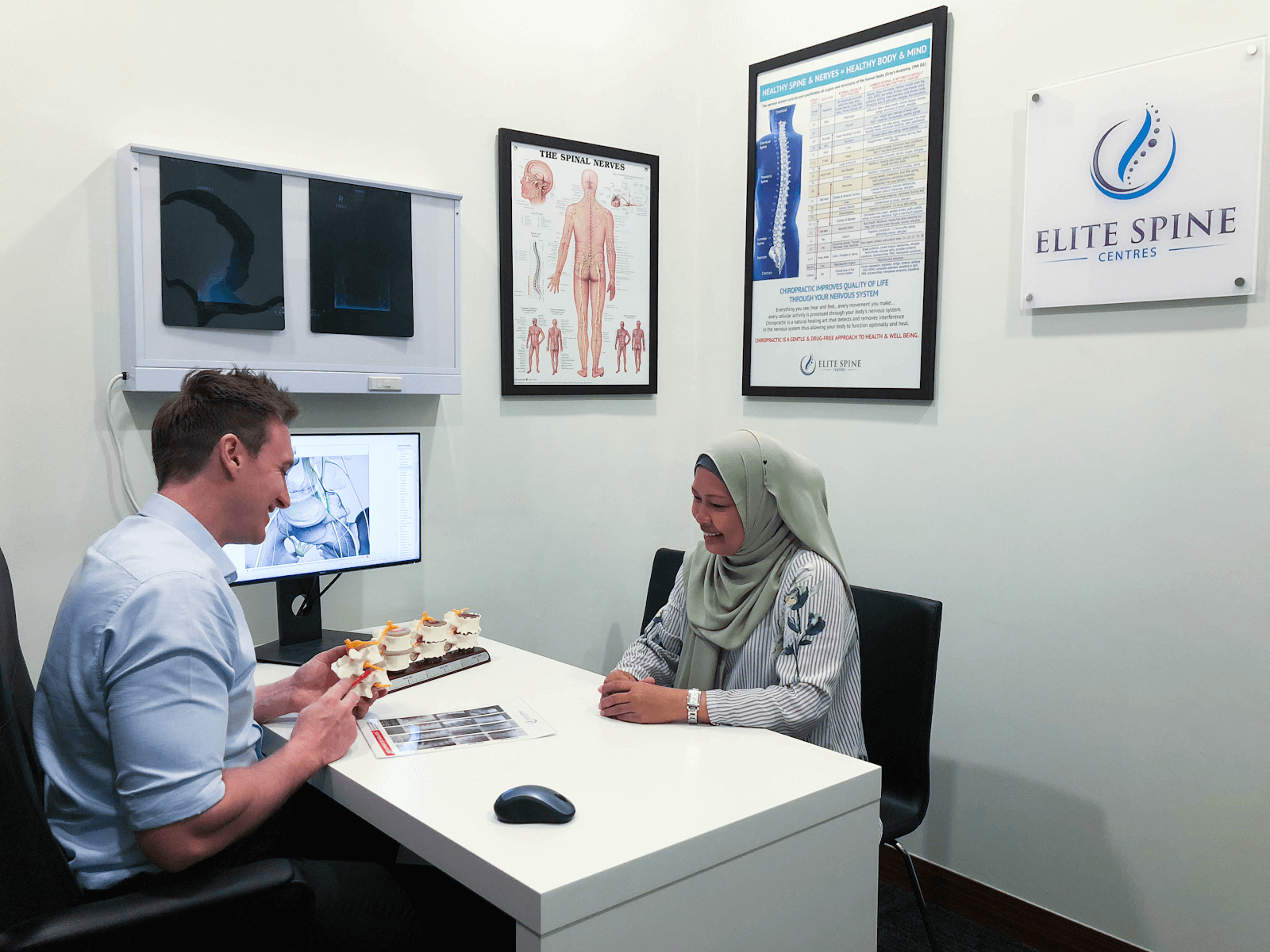
Step 1 – Initial Consultation
At Elite Spine Centres, we firmly believe in creating a low-stress, patient-centric environment.
Our Doctor of Chiropractic will review your symptoms and health history in detail to understand better what may be causing your concerns.
We will work with you to address your symptoms and concerns, ensuring that you understand your condition before proceeding with treatment.
There will be no hard sales or excessively long treatment packages – we want to work with you, not against you!
Step 2 – Spine and Body Examination
To maximise the accuracy of our diagnosis, some of these tests may specifically target the discs’ nerves to address any nerve interference or whether your back pain stems from the lumbar spine.
Additionally, imaging such as an X-ray or MRI may be required to confirm your diagnosis and help tailor your treatment recommendations.
Most of our patients will be able to receive treatment on their first session once any potential safety concerns have been ruled out!
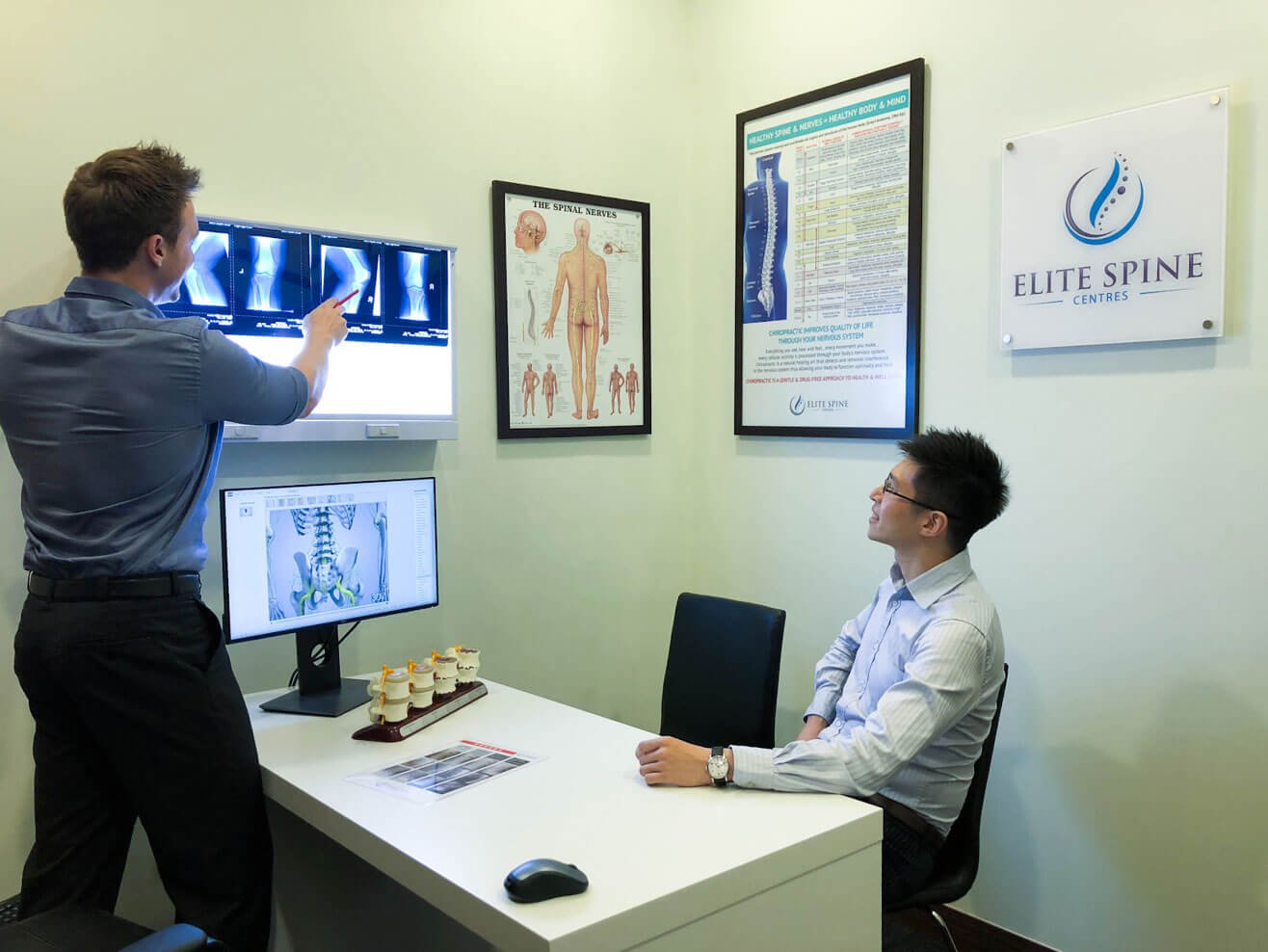
Step 3 – Doctor’s Report and Recommendations
Based on the findings, a customised plan of action will be discussed with you to help you reach your treatment goals.
Compared to the typical approach of symptoms management via medication, doctors of chiropractic can deal with the problem right at the root.
In some extreme cases where you have a progressive loss of reflexes, sensation, muscle strength, and other unusual neurological findings, you will be referred to a medical specialist to determine if immediate surgery is necessary.
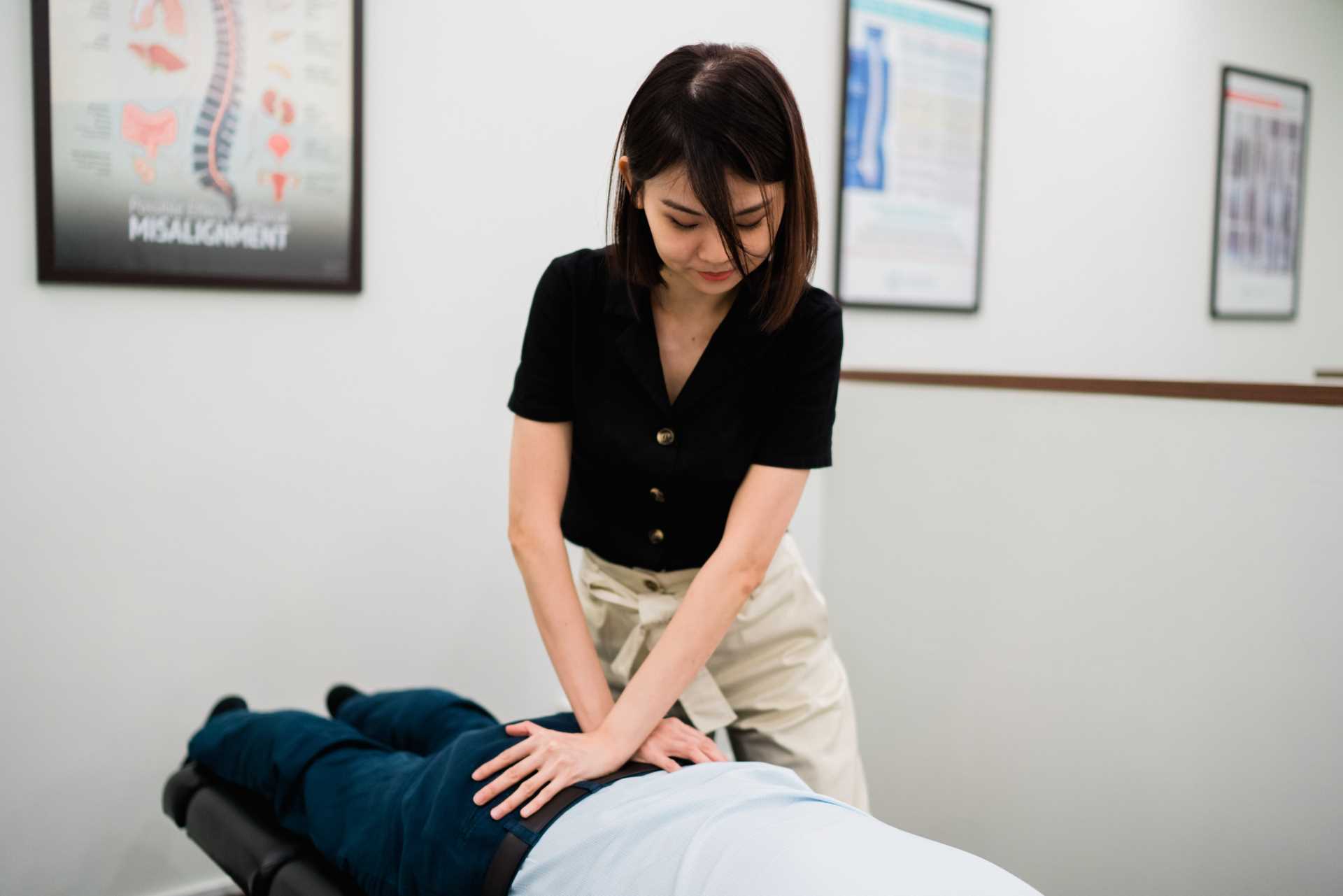
Step 4 – Holistic Chiropractic Treatment
Treatment usually involves spinal manipulation and non-surgical Spinal Decompression (NSSD) to realign your body back to its natural state, increase the range of movement, prompting an influx of healing nutrients and hydration into the disc and improve blood flow to soft tissues.
If needed, advanced therapeutic technologies may be used to complement your healing.
Your comprehensive treatment plan will also involve personalised lifestyle advice and rehabilitative exercises to prevent your condition from recurring and restore proper long-term movement patterns and posture.
This means our patients can achieve more complete recovery in a shorter time with a reduced chance of relapse than at other centres!
When to Seek Disc Pain Treatment
You should seek professional disc pain treatment if:
- Pain has persisted for more than a few weeks without improvement
- Pain is radiating down your leg or arm
- You experience tingling, numbness, or weakness in your limbs
- Daily activities such as sitting, walking, or sleeping are significantly affected
Seek immediate medical attention if you experience loss of bladder or bowel control, sudden severe weakness in both legs, or numbness in the inner thighs and groin area. These may indicate cauda equina syndrome, a medical emergency.
The earlier you seek treatment, the better your outcomes. Many cases that feel severe can recover fully with the right conservative care.
Hear What Our Patients Say
Frequently Asked Questions
Is chiropractic care safe for a herniated disc?
Yes. Chiropractic care is safe and effective for most people with a slipped or herniated disc when performed by a qualified chiropractor. At Elite Spine Centres, we always conduct a thorough assessment before beginning treatment and adapt every technique to your condition. Many patients are surprised by how gentle and immediately relieving the first session feels.
How long does slipped disc treatment take?
Recovery time varies by severity. Mild to moderate cases often see significant improvement within 4 to 6 weeks of consistent care. More severe or longstanding cases may take several months. Following your personalised plan and making lifestyle adjustments can accelerate recovery and reduce the risk of future flare-ups.
Can a slipped disc heal without surgery?
In the majority of cases, yes. Surgery is reserved for severe cases involving major neurological compromise. Most patients respond very well to conservative chiropractic treatment and spinal decompression. Research from Johns Hopkins Medicine supports that most herniated disc patients improve with conservative care including spinal manipulation and physical rehabilitation.
What happens if a slipped disc is left untreated?
Untreated disc herniation can progress and lead to complications including chronic sciatica, permanent nerve damage, persistent neuropathy in the arms or legs, or in rare cases, cauda equina syndrome with loss of bladder and bowel control. Early treatment is strongly recommended.
How many sessions will I need?
This depends on your condition, age, overall health, and how your body responds to care. Some patients notice meaningful improvement in four to six sessions. Others with more chronic presentations require ongoing care over several months. Your chiropractor will reassess regularly and adjust your plan accordingly.
What is the difference between a slipped disc, herniated disc, and bulging disc?
These terms are often used interchangeably. A bulging disc is where the disc expands beyond its normal boundary without rupturing. A herniated or slipped disc involves a tear in the outer layer, allowing the inner material to push through. Both can press on nerves and cause pain, and both can be treated effectively with the right chiropractic care.

Enjoy Our New Patient Promo for Only $88 When You Book Online!
We know that seeking chiropractic help for the first time may be overwhelming to many patients.
Hence, we prepared a special introductory package covering almost everything you need for your first two visits to our clinic!
When you book now, you’ll get our:
- Relieve pain, restore your body’s natural function & avoid surgery with our Signature Functional Correction Method (FCM)
- Get spot-on analysis and professional advice on what’s causing pain, and how to treat it with our Doctor’s Consult + Examination
Schedule your appointment right now & we’ll EVEN throw in these bonuses for FREE!
- Break down stubborn muscle knots and old scar tissue with or Doctor Directed Soft Tissue Mobilization
- Calm down & relax with our soothing ATT-300 roller massage bed
- Get a free Follow Up Consult + Xray/ MRI Review (*T&C applies)
PLUS 1 Additional Bonus Therapy (tailored specifically to you by the doctor after your consult)
- Relieve pain & inflammation with our Radial Shockwave Therapy
- Accelerate tissue healing and reduce pain with our Cold Laser Therapy
- Strengthen injured muscles and ease muscle tension with our Electric Muscle Stimulation
- Intuitive Pain Management Solution with our Super Inductive System (SIS)
*You get ALL of this for just $88
(originally priced @ $248).









